 When heart function is abnormal flecainide or propafenone are not recommended. 91% of patients taking flecainide and 55% of patients on mexiletine had a PVC reduction of ≥70%. 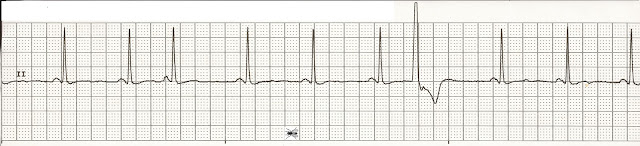
Other drugs such as flecainide or sotalol may be considered when first line therapy is ineffective. In the presence of symptoms treatment with a β-blocker or a nondihydropyridine calcium channel blocker may be the first-line therapy. A randomized placebo-controlled study showed that atenolol significantly decreased symptom frequency and PVC count. those containing monosodium glutamate) that they consider to increase the frequency of symptoms may be helpful for some people. Advice to reduce alcohol consumption, caffeinated drinks and any foods (e.g.  
For symptomatic patients lifestyle adjustment may be helpful. The long-term prognosis of frequent PVCs is considered to be benign and most of patients with frequent PVCs have normal LV function. The preferred treatment is usually reassurance and counseling of the patient with close follow-up if the patient is asymptomatic. Determining whether they are left or right sided origin is more difficult but a recent paper has demonstrated that the ratio of the S wave in V2 to the R wave in V3 (V2S/V3R) can be useful since if it is 10 000–20 000 or >10% of total heart beats over 24 hours) or if the suspicion for PVC-induced cardiomyopathy is high then an ablation might be the best form of treatment. PVCs originating from the outflow tracts are usually of left bundle branch block morphology with an inferior axis. if the PVC has a right bundle branch block morphology (positive in V1) then there is usually left ventricular origin. The standard 12 lead ECG is a very useful guide to the origin of the PVC and there is a lot of information available if you know how to interpret the trace. For example If the PVC has a left bundle branch block morphology (a negative in lead V1) then its usually a right ventricle origin. If this occurs then consideration can be given to using medical therapy or ablation to reduce the risk of a further decline in function. In people with frequent PVCs (>10,000-20,000 per 24h or >10% of the QRS complexes) or if the PVCs originate from an epicardial source then the risk of cardiomyopathy caused by the abnormal activation is increased. These patients should be screening regularly for an reduction in left ventricle function using an echocardiography. Establishing the frequency and origin of the PVCs is important to assess the risk of developing what is now becoming known as "abnormal activation cardiomyopathy" (AAC). If neither of these are present then it is likely that the PVCs will be benign and the patient is at low risk. So how should ectopic beats be evaluated and managed? I like to divide the problem into a risk assessment and an evaluation of symptoms and discussion about treatment options.įirst it is important to establish whether the PVCs are related to an underlying cardiomyopathy or ischaemic heart disease. 
Patients with ectopic beats may often be very anxious and concerned that there heart is going to stop or that they are going to have a heart attack. Sometimes the ectopic beat is an incidental finding in a patient with no symptoms. Patients may be referred because they are symptomatic with palpitations often described as "skipped or missed beats" but they may also have symptoms of shortness of breath, dizziness or poor exercise capacity. Premature ventricular contractions (PVC) also known as ventricular ectopics or ectopic heart beats are a very common problem in everyday cardiology practice. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
